Pelvic girdle pain in pregnancy
What is pelvic girdle pain?
Read below to find out about pelvic girdle pain.
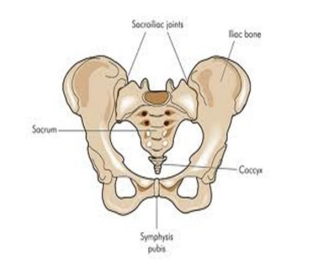
Pelvic girdle pain describes pain in and around the joints and tissues that make up your pelvic girdle. The pelvic girdle includes the symphysis pubis joint at the front of the pelvis and the sacroiliac joints (one each side) at the back of the pelvis plus many ligaments and muscles. It is a very strong structure.
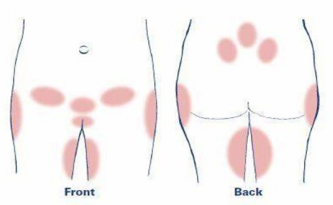
The discomfort of PGP can often be felt over these joints but can also be below your tummy, between your upper thighs or at the sides of your pelvis. It can affect one side of your pelvis or both sides. The symptoms and severity vary between women and between pregnancies in the same woman.
PGP is common with as many as 1 in 5 pregnant women reporting symptoms. Although common it is not a normal part of pregnancy and there is a lot of advice and treatment available that can help.
A small number of women may find symptoms persist after pregnancy and you can arrange further physiotherapy input to help. Causes of PGP are thought to be due to a variety of factors relating to normal pregnancy changes but sometimes there are no obvious explanations.
As pregnancy progresses your body changes shape (front loading – bump, baby, breasts) and your weight increases. Pregnancy hormones are released. These hormones affect the pelvis with the ligaments becoming stretchier, preparing it to carry a baby and for the birth itself.
All these changes alter the demands on the muscles, tissues and joints around the tummy, pelvis, hips and pelvic floor. Some support muscles are then not able to work so effectively, whilst others may overwork to help compensate.
This can result in an alteration of how your body moves with irritation and increased sensitivity of the joints and tissues around the pelvis. Equally influential to PGP are other factors such as poor sleep, stress and anxiety, previous history of back pain and constipation.
Symptoms of pelvic girdle pain (PGP)
Learn the symptoms of pelvic girdle pain and how they may affect you.
Pelvic girdle pain may cause difficulty with:
- Walking
- Standing on one leg – stairs, dressing, getting in/out of bath
- Moving legs apart – getting in/out of car
- Clicking grinding in pelvic area – you may hear or feel this
- Hip movements – turning in bed
- Some lying positions – side or back
- Some normal everyday activities
- Sexual intercourse
Top Tips
Learn top tips for supporting pelvic girdle pain.
• Try a pillow between your knees or under your bump if lying on your side
• Support/hold your bump when moving in bed
• Rather than turning over, turn under on all fours
• Turn onto your side to get in/out of bed
- Sit down to get dressed rather than standing on one leg
- Use a rucksack over both shoulders rather than carrying shopping bags in one hand
- Carry your baby/small child in front of you, rather than on one hip
- Take stairs one at a time
- Keep your knees together getting in/out of a car
- Try not to sit/stand for long periods – regularly change positions.
- Accept help, especially with other children
- Rest when you can
- Speak to a health professional if you feel you need to.
- Raise height of your chair with cushions
- Sit with legs symmetrical (not crossed or tucked under you)
- Set an alarm for 15 minutes so you regularly get up
- Try not to slump back in the chair
- Try these ideas for getting up:
- Have one foot in front of the other getting up
- Breathe out as you get up and think about squeezing your bottom muscles rather than pushing through your arms
- You could try altering your foot position to get up, for example slightly turning your feet in or out to change the muscles you are working.
- Try ice (frozen peas wrapped in a damp tea towel) over pubic bone for 10-20 minutes, up to three times per day
- For buttock pain, try a hot water bottle/wheat bag over the area
- Consider trying an elasticated tubular support/pelvic support belt during activity
- Seek advice from your GP/pharmacist as needed.
- Eat and drink adequate fibre and fluids to help avoid constipation
- When emptying your bowel keep your knees apart, consider placing your feet on a small stool and keep your tummy and breathing relaxed.
Exercise therapy
Read how exercise therapy can support pelvic girdle pain in pregnancy.
The majority of women will respond well to physiotherapy exercises and lifestyle modifications. The purpose of the exercises below is to improve the support and muscle function around your pelvis to help ease symptoms.
All of the exercises within this leaflet are safe to complete throughout your pregnancy, however as your bump gets larger you may need to adapt some of the exercise positions. It is advised that you complete the exercises in a propped up lying or side lying position to reduce potential dizziness, which can be associated with lying flat in the later stages of pregnancy. Think about using a pillow or rolled up towel to help with positioning. Complete the following exercises in a comfortable position – for example lying, sitting or standing.
- Aim for up to 10 repeats of each exercise but you may need to start with fewer and gradually build up.
- Repeat 2-3 times a day if possible.
- You should aim to practice these exercises regularly.
These exercises should not be painful but may cause some discomfort, which should settle within approximately 30 minutes. If any of the exercises cause a sharp pain or make you feel worse, stop doing that exercise for a few days and then try again. Please contact our physiotherapy service if you have any questions regarding this information.
If your symptoms are continuing despite trying the self-help advice and exercises in this leaflet, please contact our physiotherapy service. If you are having difficulty managing to complete daily tasks such as washing and dressing or going to work please consider contacting your GP to discuss pain relief.
Pelvic floor muscles
In a lying or seated position contract your pelvic floor by drawing up your front and back passages. Imagine you are trying to stop wind and at the same time trying to prevent your flow of urine. The feeling is one of ‘squeeze and lift’. It is recommended that you complete two types of pelvic floor exercises – long and short holds.
Long hold: Aim to hold this squeeze for 3 breaths in and out and build up to 10 repeats.You could also think about gently drawing in the lower part of your stomach, drawing your ‘bump’ upwards at the same time as
contracting your pelvic floor muscles.
Short hold: Aim to hold this squeeze for 1-2 seconds then relax. Aim to repeat this up to 10 times.
 In a sitting position encourage the lower part of your spine to move freely by gently arching and rounding your lower back by rocking your pelvis.
In a sitting position encourage the lower part of your spine to move freely by gently arching and rounding your lower back by rocking your pelvis.
 On all fours encourage the lower part of your spine to move freely by gently arching and rounding your lower back by rocking your pelvis.
On all fours encourage the lower part of your spine to move freely by gently arching and rounding your lower back by rocking your pelvis.
 On all fours with your knees apart to accommodate your tummy, let your arms slide along the floor/bed as far as possible. Push your bottom back and down and the chest towards the floor. Breathe out while doing the exercise.
On all fours with your knees apart to accommodate your tummy, let your arms slide along the floor/bed as far as possible. Push your bottom back and down and the chest towards the floor. Breathe out while doing the exercise.
 Place your arms across your chest. Stand up and then sit down slowly on a chair. (This can be made easier or more difficult by changing the height of the chair). Place your hands on your thighs or hips for support if required.
Place your arms across your chest. Stand up and then sit down slowly on a chair. (This can be made easier or more difficult by changing the height of the chair). Place your hands on your thighs or hips for support if required.
Stand tall with your feet slightly wider than hip-width apart. Point your toes forwards or outwards by a few degrees. Keep your chest up and your spine and neck in a neutral position.
Squat down by sitting back and bring your arms forward. Push back up through the heels, chest up, and straighten your hips.
Note:
- Keep your hips, knees and toes aligned and don't let your lower back round.
- Keep your weight evenly on your whole foot.


Stand with your feet hip-width apart and an exercise band placed around
your legs just above or under your knees with the slack taken off the band.
Squat down by moving your pelvis backwards and bending your knees. Actively push your knees against the band to keep your hips, knees and
toes aligned.


 Stand tall with your feet hip-width apart and your weight evenly on both feet. Keep your toes and knees pointing forwards. Rise up onto your toes. In a controlled manner then lower your heels back down again to return to the starting position. Note: Avoid shifting the weight towards the outer side of your forefoot during the heel raise.
Stand tall with your feet hip-width apart and your weight evenly on both feet. Keep your toes and knees pointing forwards. Rise up onto your toes. In a controlled manner then lower your heels back down again to return to the starting position. Note: Avoid shifting the weight towards the outer side of your forefoot during the heel raise.
Need more help?
Consider self referring using the link below:
If you have a new injury or problem, please look at the self help information in our advice pages. We will often complete the same exercises and share information in clinic appointments.
If you still need some more help you can self refer into our service. Please note that the NHS is currently experiencing longer than normal waits, for more information visit our waiting times page.
Click the link below for self-referal

Need more information?


